Let’s Get Started!
Reimagine your fall prevention program
The foundation of the program is the Hendrich II Fall Risk Model®, which you can use in either paper or electronic format. A highly rated, cloud-based education program will engage both novice and expert nurses as they build skills in assessing and addressing fall risk. You’ll also have access to the Hendrich Care Plans©, which reflect the latest, highest-quality evidence. The Hendrich team will offer guidance as you prioritize the care plan interventions and practices that will work best to reduce injurious falls quickly at your site of care.
Essential Program Elements
Hendrich II Fall Risk Model®
The Hendrich model has been more rigorously validated than any other fall risk tool available.
A fall assessment tool is valid when it correctly identifies persons at elevated risk of falling. The validity of a tool is proven by well-designed, peer-reviewed studies of large, representative samples of patients, including patients who fall and those who do not.
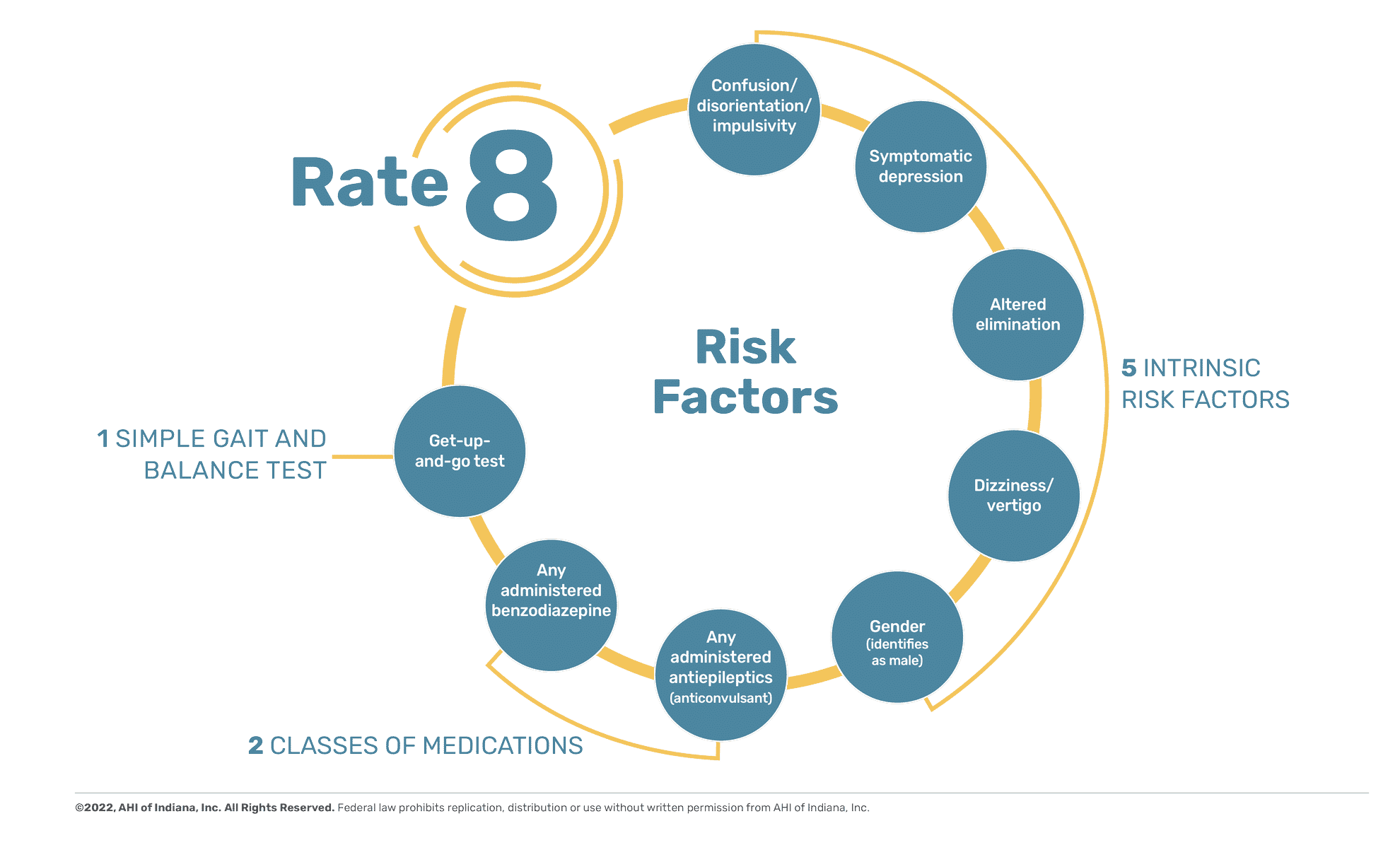
Eight risk factors, one-minute assessment
To create the model (2003), research nurses completed actual physical exams of fall and non-fall patients, using standardized assessment tools, to test more than 600 variables. Statistical modeling found 8 risk factors necessary to prevent falls.
It takes about a minute to assess your patient’s fall risk with the Hendrich model, and you can be confident that you are focusing on the risk factors that matter.
Largest study to date confirms validity of the Hendrich model
In 2020, the Hendrich team published the largest study of a fall risk model to date, with a study population of over 214,000 patients at 9 sites of care, representative of national diversity, and a study duration of three years. This study confirmed the Hendrich model’s accuracy in predicting falls and use in the electronic record.
No need for a separate tool for different clinical settings
The risk factors scientifically validated by the Hendrich model are intrinsic predictors of falling. This means that these risk factors are pathophysiological conditions that travel with the person, no matter where they are—at home, in the hospital, in the emergency department, at a clinic, etc.
The Hendrich tool can be used in the emergency department and ambulatory settings in addition to all acute care units. The only exceptions are obstetrics and pediatrics. The Hendrich team can supply more guidance on risk factors for those areas.
Hendrich Care Plans©
We built the Hendrich Care Plans© from trusted research, consultations with experts in various disciplines, and the experience of successful fall programs. Your system can quickly compare your nursing process with the care plans to select nursing interventions that will help you reduce falls at your sites of care.
You can use a building block approach. Start off with the interventions that you can quickly adopt to reduce your injurious fall rate. Our team will help you prioritize interventions based on where you are in your fall reduction efforts.
Then, when you’re ready, you can build additional interventions into your program tailored to each person’s fall risk factors. A unique benefit of the Hendrich program is that we identify the best intervention for each proven risk factor, using the highest-quality evidence and decades of experience. This makes it easy for you to construct a care plan.
We also provide the Hendrich Patient Education© resources to complement the personalized care plan. These tools help the person self-monitor and take action to reduce their fall risk factors as they transition to another environment and/or return to their home.


from novice to expert
Hendrich Cloud-Based Education©
The Hendrich Fall Prevention Program© offers unlimited, cloud-based, contact-hour-approved (.78 hours) education, with nurses teaching nurses from patient scenarios. Our interactive learning modules can help you address the pressing need to train new nurses in the current environment, where high turnover and high numbers of novice nurses are the norm.
This nursing continuing professional development activity was approved by the Midwest Multistate Division, an accredited approver by the American Nurses Credentialing Center’s Commission on Accreditation.
The Hendrich course is an efficient way for nurses to build the vital clinical and critical thinking skills necessary to predict the risk of falls and intervene effectively. Experienced nurses will appreciate the ability to “test out,” and your staff can complete short competency checks annually or every two years to sustain knowledge and skills that reduce injurious falls. We also offer a course for assistive personnel that focuses on their role in reducing falls as part of the interprofessional team.
Our education modules can interface seamlessly with your learning management system (LMS), or you can use ours to track and assign courses.
We are the only fall prevention program that offers cloud-based education for your licensed and unlicensed personnel. We’ve trained more than 150,000 clinical staff, with 99% of nurses saying they are extremely satisfied with the cloud-based learning modules.
Implementation support